Hair health depends heavily on nutrition, and the nutrient iron plays a major role in keeping strands strong and full. It helps red blood cells deliver oxygen to the cells that power hair growth, supporting healthy follicle function along the way.
Though many factors can trigger shedding, iron deficiency often slips under the radar, especially for women and those on restrictive diets.
How Iron Supports Hair Growth
Iron helps the body produce hemoglobin, a protein in red blood cells that carries oxygen. Adequate iron supports hemoglobin-mediated oxygen delivery, which is essential for rapidly dividing matrix cells in hair follicles. When iron stores drop, hemoglobin production slows. That reduces the oxygen reaching hair follicles, which can disrupt their function and weaken new growth.
Over time, chronic low iron may cause slower regrowth and noticeable thinning, making it harder for hair to bounce back to its natural fullness.
Iron Deficiency Hair Loss: What It Looks Like
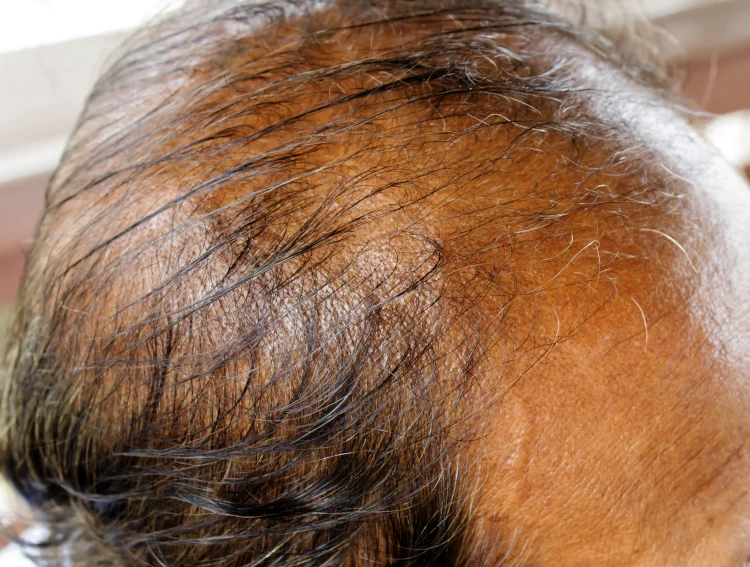
Hair loss tied to low iron usually builds up slowly. You might see more hair in your brush, on your pillow, or in the shower. Sometimes the first clue is that your hair simply looks different — less dense, more limp.
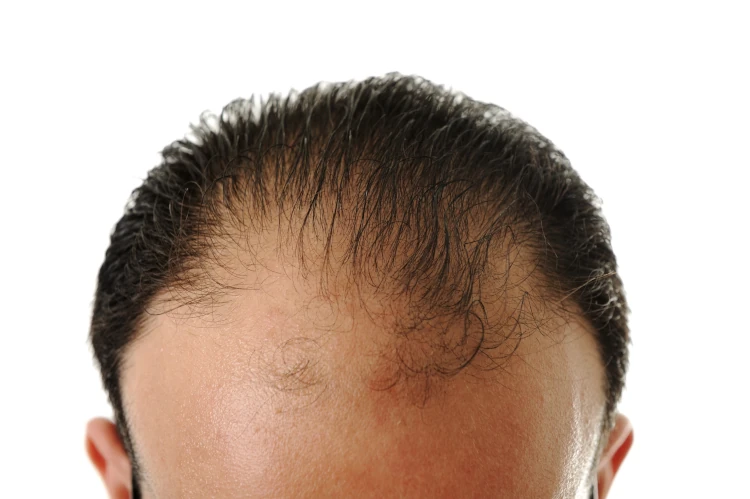
In particular, iron deficiency hair loss typically shows generalized, diffuse shedding (telogen effluvium) rather than patterned recession or a widened central part. Hair may come out more easily during brushing or washing. You might notice strands collecting faster than usual. Further, areas that shed heavily show little to no new hair growth. When you don’t see short, fuzzy baby hairs reappearing, that’s often a red flag.
These changes can resemble early signs of pattern hair loss, so visual symptoms alone aren’t always enough to know for sure.
Causes of Iron Deficiency Leading To Hair Loss

Iron deficiency doesn’t stem from just one cause. Often, it reflects a mix of diet, health conditions, and lifestyle factors. Sorting out the origin helps guide treatment.
Poor Diet
Iron comes in two forms: heme (from animal sources) and non-heme (from plants). The body absorbs heme iron more efficiently. So if you frequently skip meat or rely primarily or exclusively on plant-based foods, your iron intake may fall short.
Eating well-balanced meals with enough iron-rich foods matters, but even a healthy diet can be undermined by skipped meals or low calorie intake.
Heavy Menstruation
Monthly blood loss from periods can gradually drain iron stores, especially when cycles are heavy. Over time, this depletion may lead to fatigue, weakness, and increased hair shedding.
Because the symptoms build slowly, many don’t connect them to iron loss right away.
Pregnancy
Pregnancy increases the body’s iron demands significantly. Without enough intake through food or supplements, it’s easy to become deficient. Further, people often blame hair shedding after childbirth on hormones, but low iron can also make recovery harder and prolong the regrowth phase.
Most postpartum shedding is hormonal telogen effluvium and resolves within six to 12 months; iron deficiency, if present, can delay regrowth.
Digestive Conditions
Certain gut disorders — such as Crohn’s or celiac disease — can block the body from absorbing iron effectively, even if your diet is on point. When your body isn’t absorbing iron, hair follicles lose their steady supply of oxygen and nutrients.
Weight Loss
Acute weight-loss diets may provoke telogen effluvium via calorie and protein deficits. True iron deficiency is more common after bariatric surgery, heavy menstrual bleeding, gastrointestinal loss, or malabsorption.
Ways To Combat Hair Loss Caused By Iron Deficiency
To address iron deficiency, eating more iron-rich foods is a great place to start. Red meat, lentils, spinach, and fortified cereals can help restore iron levels gradually. Pairing these foods with more than 75 milligrams of vitamin C can increase non-heme iron absorption threefold.
If dietary changes aren’t enough, iron supplements may be needed. It’s a good idea to check with a doctor first to avoid taking more than your body requires. Begin only after confirming deficiency; the typical oral dose is 40-65 milligrams of elemental iron on alternating days. Monitor ferritin every eight to 12 weeks. Over-supplementation can cause iron overload or obscure cardiac and thyroid lab results.
Recovery doesn’t happen overnight, but consistent iron intake often brings steady improvements in energy, mood, and hair density.
Diagnosing Iron Deficiency as the Cause of Hair Loss
If you think iron might be the issue, talk to your doctor about a blood panel. These tests can help confirm whether your hair loss ties back to low iron.
Key lab values that can help clarify the picture include:
- Serum ferritin measures iron storage in the body and is one of the most sensitive indicators of iron deficiency. Low levels often indicate depleted iron reserves, even before anemia develops. Most dermatologists begin treatment when ferritin is less than 30-40 micrograms per liter, even without frank anemia.
- Hemoglobin gauges the amount of oxygen-carrying protein in red blood cells. A drop in hemoglobin can point to anemia, which is closely linked to fatigue and hair thinning.
- Iron saturation and total iron-binding capacity (TIBC) tests help assess how well iron is transported in your bloodstream. These values offer insight into whether your body has enough iron to meet cellular needs.
This kind of bloodwork helps pinpoint whether iron is the likely cause. That way, you’re not guessing or jumping into treatments that won’t help.
That said, iron isn’t the only possible trigger. Thyroid issues, autoimmune conditions, stress, and genetics can all play a role in hair loss. That’s why a full diagnosis from a medical professional matters. If you self-diagnose and you’re incorrect, you may continue to experience hair loss, as well as fail to address its underlying cause.
Treatment Options Beyond Supplements
Restoring iron levels is the foundation of treatment, but in some cases, it takes more to get hair growing again. Treatments like topical minoxidil can reawaken sluggish follicles and encourage regrowth.
Early studies suggest platelet-rich plasma therapy may improve hair density in TE and androgenetic alopecia, but data are limited and treatment is considered off-label. Surgical hair restoration is deferred until ferritin is corrected and shedding stabilizes; otherwise, graft survival is poor.
A personalized consultation helps determine whether this route is worth considering. Before-and-after photos give a clearer sense of what’s achievable when iron levels are restored and additional treatments are used to support regrowth.
Treatment costs can vary depending on the extent of hair restoration and the expertise of the clinic. Getting a clear quote ahead of time helps you avoid surprises and plan with confidence.